
Article: Friday, 19 March 2021
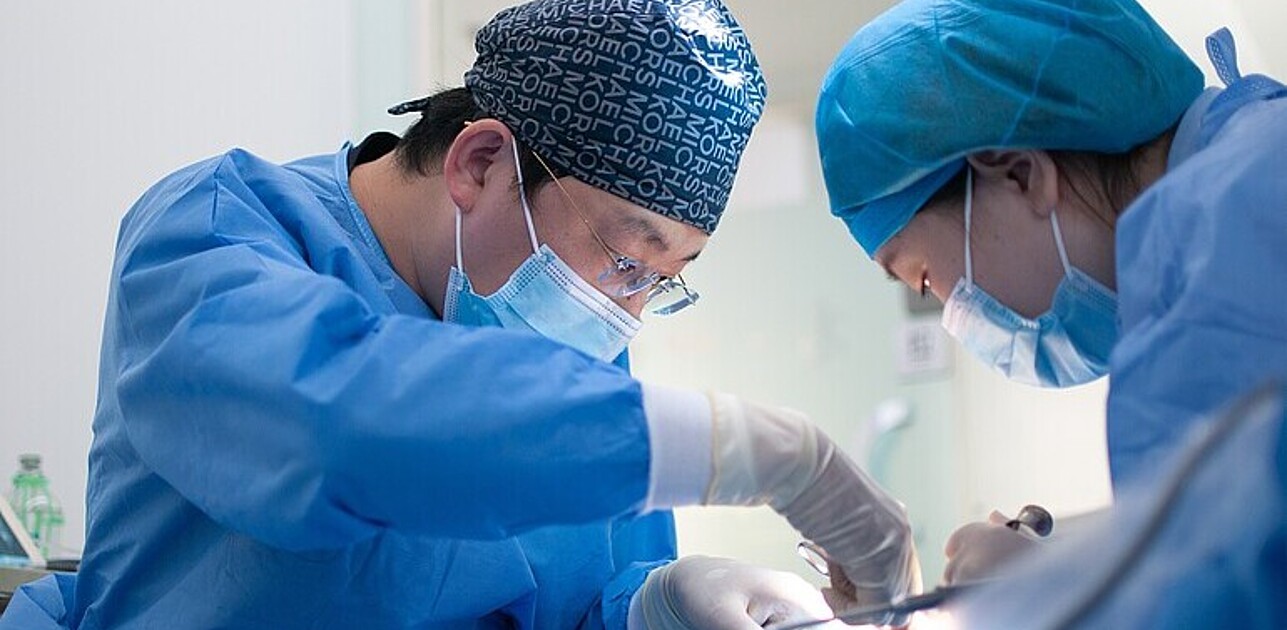
Healthcare systems are in the frontline of the battle against the COVID-19 pandemic. In most countries, they are operating at near full capacity. Healthcare staff are are working relentlessly under heavy psychological and physical distress. Their feelings of failure as they care for such sick patients with such high death rates are like nothing they have experienced before. Research that helps hospital managers mitigate the psychological and operational impact of negative experiences of medical staff, such as patient deaths, has been carried out by Dr Ioannis Fragkos of Rotterdam School of Management, Erasmus University (RSM), Dr Emmanouil Avgerinos of IE Business School, Madrid and Prof. Bilal Gokpinar of UCL School of Management, London.
Failure – any unwelcome outcome – is commonplace in many contexts that involve knowledge work. But how does failure affect subsequent performances for skilled workers in healthcare? How do healthcare workers feel when patients die, and how does this affect the way they continue with their work?
Dr Fragkos, an associate professor in RSM’s department of Technology and Operations Management, explained: “First, we wanted to improve our understanding of the drivers of efficient and inefficient surgical operations.” The operations they looked at were complicated but common procedures such as coronary artery bypass grafting and tumor removals. “Efficient operations are those that are successfully carried out in a short amount of time, thereby contributing to the provision of a high level of healthcare and a fast turnover of patients.”
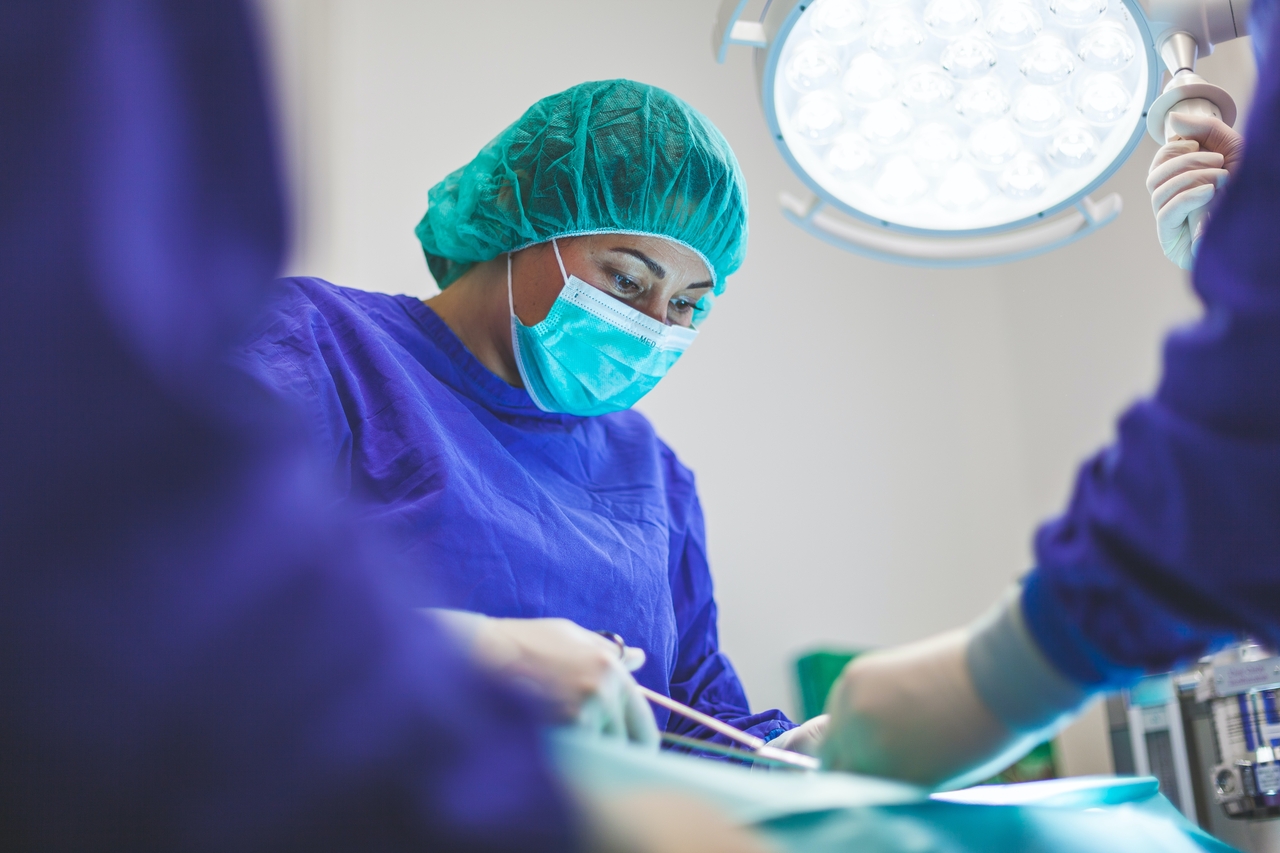
“Once we realised the importance of familiarity within and among the team members, and the importance and impact of the experience of failure after a team task, we wanted to explore whether the positive effect of familiarity can mitigate the short-term negative effects of failure.” This question led the researchers to explore strategies for forming teams based on their familiarity – which they defined as the number of interactions the team members had had with each other in the past.
Before the pandemic, there was a short series of studies about the effect of failure on subsequent performance in cardiac surgery, and the effects of hierarchy and failure on team productivity. These studies gathered and examined more than 4,000 detailed cases from cardiac surgery operations; the severity of each operation, the team members involved, the outcome, and how long each patient stayed in hospital.
The study of Dr Fragkos and his colleagues suggests that when surgical teams have negative experiences – such as the death of a patient that they have operated on – they experience negative emotions which reduce the teams’ performances on subsequent operations. Specifically, patients operated on by a team that recently experienced another patient’s death need more in-hospital recovery time.
With hospital beds being a limited resource, hospital managers should be alert to this hidden impact of patient deaths. Not only do patients’ deaths affect healthcare staff mentally; they also lead to reduced performance during subsequent surgeries on other patients, which then extends in-hospital stays of those other patients.
Put into numbers, the study suggests that just one recent patient death experience for a surgical team can increase in-hospital stays for the teams’ subsequent patients by 44 per cent (which translates to around 4.6 days). The consequences could be significant for the deployment of a hospital’s critical resources.
Dr Fragkos and his colleagues also observed that teams in which the members are very familiar with each other are more resilient after experiencing failure. This means that assigning tasks to teams already familiar with each other can mitigate possible impediments to productivity after patient deaths.
Dr Fragkos and his colleagues used a simulated model to compare a ‘normal’ rotation policy for team members against a policy that avoids pairing the lead surgeon with less familiar team members. The results showed an almost 30 per cent reduction in the length of hospital stay for patients operated on by a lead surgeon that had recently experienced failure if the surgeon was paired with a familiar team. The hospital data studied in the simulation implied a reduction of three days in the total length of stay per patient. Such a policy – of pairing lead surgeons with teams that are familiar to them – means managers can support employees in moving forward after failure. But they can also achieve a higher turnover through the hospitals beds, and ultimately increase the hospital’s throughput.
Although the performance of surgical teams is subsequently lowered by patient deaths induced by surgery, such failures can have an often overlooked positive from the point of view of performance. When Dr Fragkos and his colleagues studied the long-term effect of surgery-induced patient deaths, he found that experiencing failure leads to an improvement in the quality of tasks executed and promotes learning for healthcare teams.
After analysing hospital data, the researchers found that the healthcare team’s improved learning as a result of past failures appears to reduce the length of stay of its subsequent patients by a total of 168 days per month – which could translate into 16 additional admissions per month.
Healthcare managers who recognise how failures improve productivity in the long term will still see failures as learning opportunities. Such leaders understand that team members who together experience failures can develop more meaningful familiarity with each other, which ultimately improves their productivity.
At the same time, however, effective leaders should protect the members of healthcare teams and their organisation from the psychological effects – and the operational ramifications – that come in the aftermath of the death of a patient. By keeping teams as stable as possible when times are hard, which can be difficult but not impossible, leaders can mitigate short-term negative effects of failure and harness its positive aspects in the long term.

The paper has been published in the Journal of Operations Management (STAR) under the title The effect of failure on performance over time: The case of cardiac surgery operations.


Science Communication and Media Officer
Rotterdam School of Management, Erasmus University (RSM) is one of Europe’s top-ranked business schools. RSM provides ground-breaking research and education furthering excellence in all aspects of management and is based in the international port city of Rotterdam – a vital nexus of business, logistics and trade. RSM’s primary focus is on developing business leaders with international careers who can become a force for positive change by carrying their innovative mindset into a sustainable future. Our first-class range of bachelor, master, MBA, PhD and executive programmes encourage them to become to become critical, creative, caring and collaborative thinkers and doers.
