
Article: Thursday, 12 March 2020
One of the most urgent challenges that society faces is bearing the rising health care costs of an aging global population. We could deal with it using technological innovation in the techniques we use for treatment. But whereas a hospital’s decision to adopt an innovation can be straightforward, the implementation process is often complicated. Therefore Jan van Schaik, a surgeon at Leiden University Medical Center (LUMC) and Dr Merieke Stevens of Rotterdam School of Management, Erasmus University (RSM) studied the implementation of new medical technologies as a way to increase the effectiveness of care. They focused on aortic disease, which affects an increasing number of people globally. Their research demonstrated that team learning is supported by factors of relational and cognitive embeddedness, which in turn enables the team to achieve the goals it sets for itself. This is the first time that the role of these factors during the implementation of a complementary technology for low volume, high complexity care has been studied in healthcare.
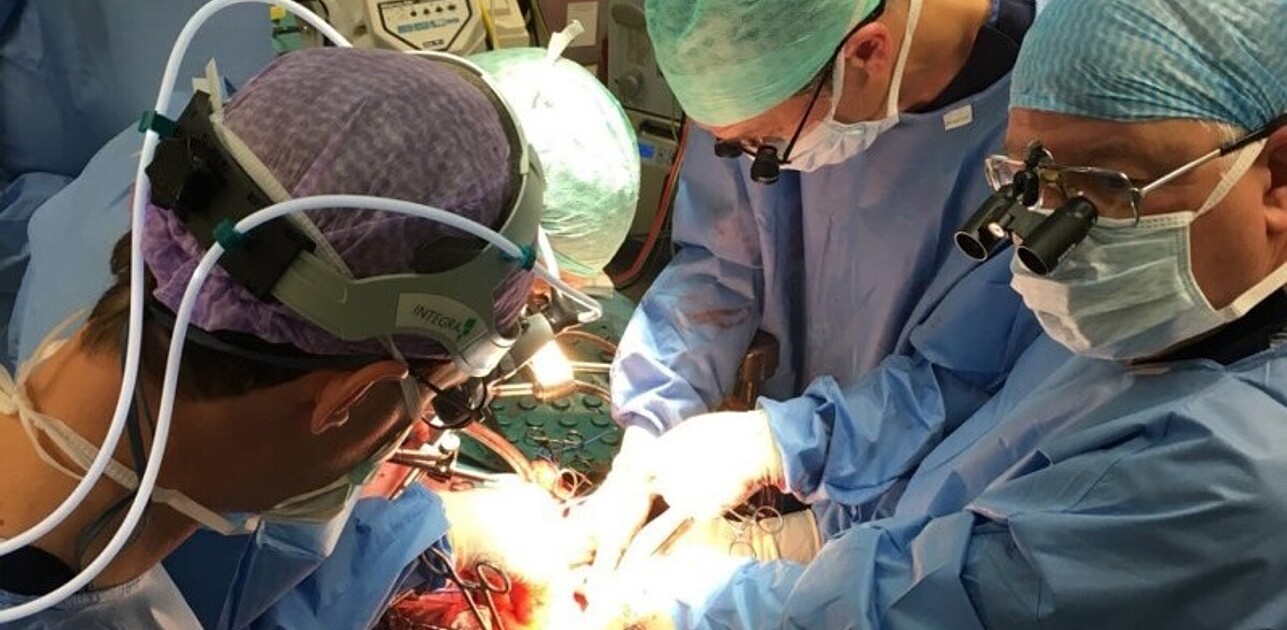
Researchers often study medical teams delivering high volume, low complexity treatments. Stevens and Van Schaik, the researchers here, had the opportunity to study the implementation of a new and complementary technology for a low volume, high complexity treatment. They studied complex endovascular aorta reconstruction. This procedure involves accessing the aorta via the arteries in the groin and arm, instead of surgically opening the abdomen and thorax.
Their research focused on the multidisciplinary team of medical professionals working on complex aorta treatment. The new technology posed huge challenges for them because the technology could not be tested; was judged and validated only internally (by the team itself); and could only be learned on the job. Whereas thoracic and vascular surgeons are responsible for open reconstruction of the aorta, the new technology also required expertise from interventional radiologists familiar with minimally invasive techniques, who therefore became important team members. Furthermore, since such complex endovascular treatment employs a custom-made stent designed to exactly fit each patient’s anatomy, the supplier of the stents also became much more embedded in the treatment team. This shift in the professional composition of the team’s members brought another organisational challenge.
Van Schaik and Stevens’ research focused on the goals that the treatment team had set for itself, rather than more general (and quantifiable) goals such as blood loss or days spent in hospital. Jan van Schaik, one of the lead surgeons on the programme, stressed this by asserting that outcomes such as reduced blood loss or minimised stay in hospital critically depend on team functioning.
The team set goals to:
Each member of the 19-strong team was interviewed in depth, and information gathered from the interviews was combined with medical data from all of the patients treated within the programme between 2013 and 2017.
The study showed evidence that the team achieved goals 1, 2 and 3. During the final stage of the study, there were initial indications that it also reached goal 4.
Despite the importance of the technical skills of medical professionals on the team, the researchers’ analysis revealed that it was relational and cognitive embeddedness factors that ultimately enabled the whole team to reach its goals. These were the relational embeddedness factors comprising frequent, formal and informal communication, and mutual trust – as well as cognitive embeddedness factors – comprising shared norms for roles and behaviour, shared goals during treatment in the operating theatre, and a very strong sense of shared responsibility. These all led to the team being able to build its capabilities.
The healthcare system in the Netherlands (as elsewhere) is under huge stress, with rapidly changing technology providing both an opportunity as well as a threat; the system is in need of improvement.
This study demonstrates that investments in relational and cognitive embedding can help healthcare teams to achieve their goals while dealing with high demands for their services.
An example of the co-operation and communication in the team came through in the results of the study. Here’s a scrub nurse’s story that came from one of the in-depth interviews:
“A vascular surgeon came to us to show a stent, and its markers. Normally you don't get to see those things that cost I don't know how many euros. So, I thought: “That is what they are talking about, and that's how it's folded up, and if they do this, it deploys like that.” It was so much more insightful for me from then on. Before, I would simply get lost at one point. Now I finally understood what they were trying to do and why they have to be concentrated.”
While the scrub nurse did not need this technical knowledge to perform their task, it enhanced their overall ability to support the team. Healthcare can be improved when teams pay attention to relational and cognitive embeddedness factors. Medical personnel are under huge strain and recognising that time is needed for embedding teams is necessary to improve medical outcomes.

Read the article: M. Stevens & J. van Schaik (2020). Implementing new technologies for complex care: The role of embeddedness factors in team learning. Journal of Operations Management (STAR), 66 (1-2), 112-134. Digital Object Identifier: 10.1002/joom.1034


Science Communication and Media Officer
Rotterdam School of Management, Erasmus University (RSM) is one of Europe’s top-ranked business schools. RSM provides ground-breaking research and education furthering excellence in all aspects of management and is based in the international port city of Rotterdam – a vital nexus of business, logistics and trade. RSM’s primary focus is on developing business leaders with international careers who can become a force for positive change by carrying their innovative mindset into a sustainable future. Our first-class range of bachelor, master, MBA, PhD and executive programmes encourage them to become to become critical, creative, caring and collaborative thinkers and doers.
